VoC for Healthcare
An Agentic Voice of Customer (VoC) Intelligence that transforms patient and member experience across every care journey.
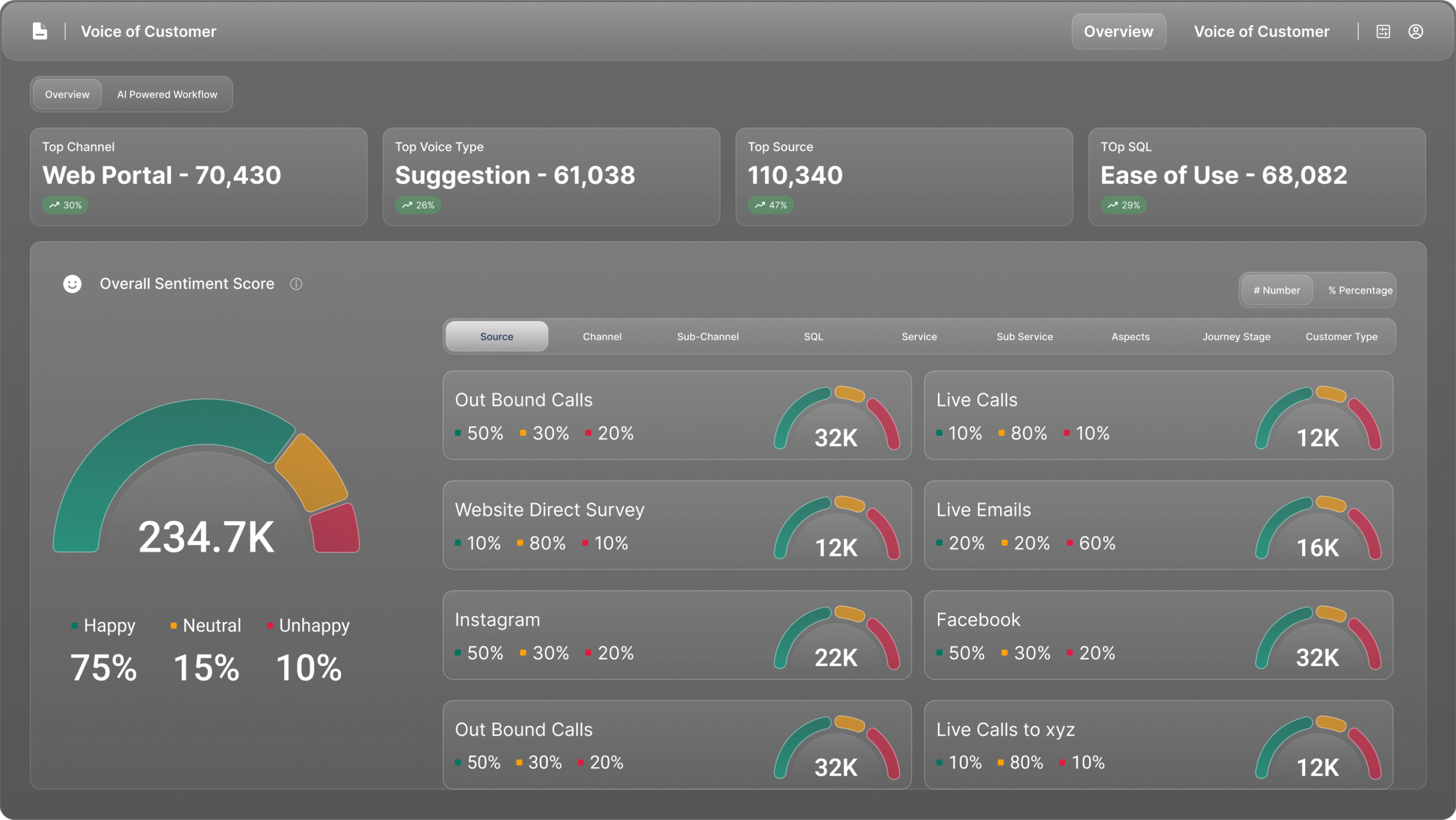
Why Healthcare Organization Struggle During Experience Breakdowns
From patient signals to clinical and administrative action, healthcare systems lack a unified intelligence layer to manage experience, access, and
compliance at scale.
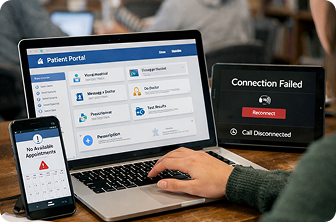
58%
Digital Experience Breakdowns
Patient portals, appointment booking, telehealth failures.
35%
Complaints
Billing disputes, claim denials, appointment delays, care coordination gaps.
3-7 Days
Slow Issue Resolution
High AHT, multiple handoffs, manual case reviews.
<10%
Experience Blind Spots
Calls, portal messages, surveys, reviews, social mostly unstructured.
<1100%
Interaction Volume Spikes
System outages, care delays, public health events overwhelm support.
Healthcare Doesn’t Need More Data. They Need Faster Care Action
Legacy Healthcare VoC
5-10% survey response rate
Feedback captured only after dissatisfaction or escalation.
No real-time visibility into patient issues.
Slow, manual grievance handling.
Typical AI Tools
Basic sentiment and keyword tagging.
Healthcare Doesn’t Need More Data.
No automated triage or intervention.
Issues resolved case by case Scenario.
Agentic VoC Intelligence
100% feedback capture across care journeys.
Real-time reasoning for Care, Operations, and Compliance teams.
Auto-triage, intelligent routing, and service recovery.
AI-driven insights at healthcare scale across facilities, service lines.
HIPAA-ready, auditable workflows with traceable triage, routing.
Botminds Agentic VoC Intelligence for Healthcare
AI agents that capture, understand, and act across the full patient journey.
100% Capture
Capture every patient signal across channels. Zero blind spots.
Deep Understanding
Detect intent, urgency, sentiment, care risk, and billing sensitivity.
Smart Clustering
Auto-group themes and issues. Prioritized by risk and volume.
Actionable Insights
Daily clarity for Care Delivery, Operations, and Admin teams.
Autonomous Action
Auto-route, escalate, and track closure end to end.

Calls, portal messages, chats, grievances, claims inquiries

Appointment delays, care gaps, discharge issues, denial confusion, billing disputes

Clinic-level hotspots, recurring grievances, high-risk patient clusters

Top drivers, root causes, turnaround trends, department-wise breakdowns

Measure Patient
& Operational Impact
From feedback to patient satisfaction, complete intelligence for modern healthcare VoC operations.


Faster, Frictionless Resolution
Patient and member issues resolved without unnecessary delays.

Lower Cost-to-Serve
Reduced call volumes, fewer repeat contacts, less manual handling.

Streamlined Complaint Handling
Captured, understood, and routed instantly.

Stronger Communication
Clear, proactive updates on appointments, care, and billing.

Improved Trust & Loyalty
Patients and members feel heard, supported, and cared for.

Robust Regulatory Compliance
Consistent, auditable handling of complaints and sensitive cases.
How it works
Enterprise-grade intelligence in five seamless steps
Listen
Capture patient and member signals across digital, clinical, and administrative touchpoints.
Understand
Identify issue type, care context, urgency, and risk.
Decide
Prioritize actions using SLAs, care impact, and regulatory rules.
Act
Auto-route cases, trigger interventions, and notify patients or members.
Learn
Continuously improve care experience, access, and operational outcomes.
Omni - Channel Ingestion
 Voice
Voice.png) Chat
Chat Email
Email Social Media
Social Media Video
Video Surveys
SurveysCognitive processing layer
 LLM Gateway
LLM Gateway
Multi-agent Cognitive Engine
 Listening
Listening Understanding
Understanding Reasoning
Reasoning Action
Action Narrative
Narrative Continuous Learning
Continuous LearningAutonomous Workflows
 Self-healing Workflows
Self-healing Workflows Auto-triage & Routing
Auto-triage & Routing Cross-team Escalations
Cross-team EscalationsExperience Intelligence
 Dashboards
Dashboards Alerts & Briefs
Alerts & Briefs Analytics
Analytics Co-pilot
Co-pilot Cockpit
Cockpit Decision & Action APIs
Decision & Action APIsFrom Signals to Operational Action
Closed-Loop
Passenger
Experience
Engine

Care Operations
Fewer Manual Follow-ups → Higher Operational Efficiency

CEO/COO
Improved Care Coordination → Stronger Organizational Confidence.

Compliance & Privacy Teams
Early Risk Detection → Reduced Regulatory Exposure

Patients / Members
They feel informed → Trust increases

Patient Services / Contact Centers
Lower workload → Faster Case Resolution

Digital / Experience Teams
Unified Feedback → Better Care Journey Improvements
Enterprise-grade
Everything

ISO 27001:2013 Certified

SOC 2 Type II Certified

GDPR Compliant